外国人患者さんの受診

通訳 -
電話 通訳 サービス誰 でも電話 通訳 サービスを使 うことが できます。
毎日 いつでも無料 です。使 いたいとき、病院 の職員 に頼 んでください。
以下 の外国語 を通訳 することが できます:①
英語 ②中国語 ③スペイン語 ④ポルトガル語 ⑤韓国語 ⑥ベトナム語 ⑥タイ語 ⑦ロシア語 ⑨ネパール語 ( ) ⑩フランス語 ( ) ⑪タガログ語 ( ) ⑫インドネシア語 ( ) ⑬ドイツ語 ( ) ⑭イタリア語 ( ) ⑮マレー語 ( ) ⑯クメール語 ( ) ⑰ミャンマー語 ( ) ⑱モンゴル語 ( ) ⑲シンハラ語 ( ) ⑳ヒンディー語 ( ) ㉑ベンガル語 ( ) ) ㉒ウルドゥー語 ( ) ) 難 ( ) しい日本語 ( ) が多 ( ) いですから、家族 ( ) や友人 ( ) は通訳 ( ) を しません。
権利 ( ) とお願 ( ) い-
「
患者 ( ) さんの権利 ( ) 」と「患者 ( ) さんへのお願 ( ) い」「
患者 ( ) さんの権利 ( ) 」個人 ( ) の尊厳 ( ) 病院 ( ) は あなたの気持 ( ) ちや考 ( ) え方 ( ) を大切 ( ) に します。平等 ( ) で最良 ( ) の医療 ( ) を受 ( ) ける権利 ( ) 患者 ( ) さんは誰 ( ) でも倉敷中央病院 ( ) で行 ( ) える一番 ( ) 良 ( ) い治療 ( ) を受 ( ) けることが できます。インフォームド・コンセントと
自己 ( ) 決定権 ( ) ■
病院 ( ) は病気 ( ) や治療 ( ) や検査 ( ) について あなたに わかりやすく説明 ( ) します。説明 ( ) を聞 ( ) いて、よく理解 ( ) してから、治療 ( ) や検査 ( ) を選 ( ) ぶことが できます。■ あなたは
治療 ( ) を受 ( ) けるか受 ( ) けないかを決 ( ) めることが できます。「治療 ( ) や検査 ( ) を受 ( ) けません」と言 ( ) うことも できます。■ あなたは ほかの
病院 ( ) で病気 ( ) や治療 ( ) について質問 ( ) することが できます。■
研究中 ( ) の新 ( ) しい薬 ( ) を使 ( ) ったり、新 ( ) しい治療 ( ) を したりするとき、あなたに詳 ( ) しく説明 ( ) します。
あなたは説明 ( ) を よく聞 ( ) いてから、新 ( ) しい薬 ( ) を使 ( ) うかどうか、新 ( ) しい治療 ( ) を するかどうかを決 ( ) めることが できます。診療 ( ) 情報 ( ) の提供 ( ) を受 ( ) ける権利 ( ) あなたは
病院 ( ) から自分 ( ) の治療 ( ) の情報 ( ) を求 ( ) めることが できます。プライバシーの
保護 ( ) と秘密保持 ( ) の権利 ( ) 病院 ( ) は あなたの プライバシーを守 ( ) ります。
病院 ( ) は、あなたの情報 ( ) を病院 ( ) の中 ( ) だけで使 ( ) います。 あなたに確認 ( ) することなく、あなたの情報 ( ) を他 ( ) の人 ( ) に伝 ( ) えません。「
患者 ( ) さんへの お願 ( ) い」- あなたの
体調 ( ) や病気 ( ) について正 ( ) しく教 ( ) えて ください。 治療 ( ) や検査 ( ) を するとき、 あなたも意見 ( ) や気持 ( ) ちを教 ( ) えて ください。治療 ( ) のとき、病院 ( ) の規則 ( ) を守 ( ) って ください。病院 ( ) に たくさんの患者 ( ) さんが います。安心 ( ) して受診 ( ) が できるように協力 ( ) して ください。病院 ( ) に研修医 ( ) 〈=研修 ( ) を受 ( ) けている医師 ( ) 〉が います。協力 ( ) して ください。病院 ( ) に医師 ( ) や看護師 ( ) の勉強 ( ) をする学生 ( ) が います。学生 ( ) は病院 ( ) の中 ( ) を見 ( ) たり、病院 ( ) の仕事 ( ) を勉強 ( ) したり しています。学生 ( ) について意見 ( ) が あるとき、病院 ( ) の職員 ( ) に言 ( ) って ください。
- あなたの
受診 ( ) -
準備 ( ) します1)
家 ( ) の近 ( ) くの病院 ( ) に行 ( ) きます。
2)その病院 ( ) で紹介状 ( ) (倉敷中央病院 ( ) に わたす手紙 ( ) )を もらいます。
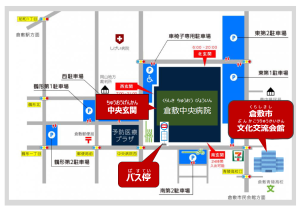
3)その病院 ( ) で倉敷中央病院 ( ) の予約 ( ) を します。倉敷中央病院 ( ) に行 ( ) きます
救急 ( ) -
受診 ( ) します毎日 ( ) 24時間 ( ) 受診 ( ) することが できます。◆注意◆
PM6:00から次 ( ) の日 ( ) のAM9:00までの 間 ( ) は、診療費 ( ) と一緒 ( ) に 7700円 ( ) も払 ( ) います。
出産 ( )
医療費 ( ) -
お
金 ( ) を払 ( ) います次 ( ) の 1~3で お金 ( ) を払 ( ) うことが できます。現金 ( ) - デビットカード
- クレジットカード(DC / UFJ / NICOS / VISA / MASTER / MUFG / JCB / DinersClub / AmericanExpress / DISCOVER)